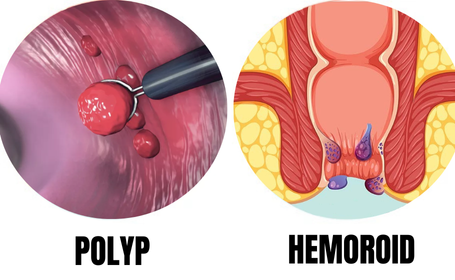
What Are the Differences Between Anal Polyps and Hemorrhoids?
💡 Quick Answer
Anal polyps and hemorrhoids are not the same condition: anal polyps are tissue growths from the lining of the anal canal or rectum, while hemorrhoids are enlarged vascular cushions or swollen veins in the anal region. They may cause similar symptoms such as rectal bleeding, itching, mucus discharge, a lump sensation, or discomfort, so self-diagnosis is often unreliable. Hemorrhoids are usually related to pressure, constipation, straining, pregnancy, or prolonged sitting. Anal or rectal polyps may arise from mucosal overgrowth, chronic irritation, inflammation, or colorectal polyp disease. Some polyps are harmless, while others may need removal and pathology review. Hemorrhoids are commonly treated with lifestyle changes, office procedures, laser treatment, or surgery depending on severity. Persistent bleeding, rapid growth, pain, bowel habit changes, unexplained weight loss, anemia, or a new anal lump should be evaluated by a proctology specialist.
What Are Anal Polyps and Hemorrhoids?
Anal polyps and hemorrhoids are often confused because both can appear as a lump, fullness, bleeding, itching, or irritation around the anus. However, they are different conditions with different tissue origins and different follow-up needs.
Anal polyps are tissue protrusions that arise from the mucosal lining of the anal canal or rectum. Some are inflammatory or fibroepithelial growths, while others may be related to colorectal polyp disease and require endoscopic evaluation. Hemorrhoids, also called piles, are enlarged vascular cushions or swollen veins inside or around the anus and lower rectum.
In ICD-10 coding, hemorrhoids are generally classified under K64. Anal and rectal polyps may be coded differently depending on their exact location and pathology; rectal polyps may fall under K62.1, while colon polyps may be classified under K63.5. The exact code depends on the physician’s diagnosis and pathology results.
For more information on hemorrhoid care, you may also review hemorrhoids treatment.
What Symptoms Can Anal Polyps and Hemorrhoids Cause?
Anal polyps and hemorrhoids can overlap in symptoms, but the pattern is often different. Hemorrhoids more commonly cause bleeding, itching, swelling, prolapse, and discomfort. Polyps may be silent, or they may cause bleeding, mucus discharge, a feeling of fullness, or a visible/palpable tissue protrusion.
Symptoms that may occur in both conditions
- Bright red rectal bleeding
- Anal itching or irritation
- Mucus discharge or wetness
- A lump or protrusion near the anus
- Feeling of fullness or incomplete cleaning
- Discomfort during bowel movements
Symptoms more suggestive of hemorrhoids
- Bleeding during or after bowel movements
- Prolapse that comes out with straining
- Painful swelling in thrombosed external hemorrhoids
- Itching due to moisture and irritation
- Symptoms triggered by constipation, pregnancy, heavy lifting, or straining
Symptoms that may raise concern about a polyp or another condition
- Persistent bleeding not clearly linked to straining
- Change in bowel habits
- Unexplained anemia
- Unexplained weight loss
- Family history of colorectal cancer or polyps
- A lesion that grows, changes shape, or bleeds easily
Why Do Anal Polyps and Hemorrhoids Occur?
Anal polyps and hemorrhoids form through different mechanisms. Hemorrhoids are mainly vascular and pressure-related. Polyps are tissue growths from the mucosa. This difference explains why their treatment and follow-up are not the same.
How do anal polyps form?
Anal or rectal polyps may form because of mucosal overgrowth, chronic irritation, inflammation, previous fissure-related changes, or colorectal polyp disease. Some polyps are benign inflammatory tissue growths. Others, especially colorectal adenomatous polyps, may have precancerous potential and require removal and pathology review.
How do hemorrhoids form?
Hemorrhoids occur when vascular cushions in the anal canal enlarge, swell, or prolapse. Risk factors may include constipation, straining, pregnancy, prolonged sitting on the toilet, heavy lifting, obesity, and aging. NIDDK lists anal itching and rectal bleeding among possible hemorrhoid symptoms, while NHS notes constipation, pushing too hard during bowel movements, pregnancy, heavy lifting, getting older, and being overweight as factors that make hemorrhoids more likely.
What Can Be Done at Home, and What Should Be Avoided?
Home care can help reduce irritation and constipation-related pressure, especially if hemorrhoids are present. However, home care cannot reliably distinguish a polyp from a hemorrhoid, and it cannot determine whether a polyp needs removal.
Supportive steps at home
- Increase fiber intake gradually.
- Drink enough water unless medically restricted.
- Avoid straining during bowel movements.
- Limit time spent sitting on the toilet.
- Use gentle cleaning with water instead of harsh wipes.
- Avoid scratching the anal area.
- Track bleeding, lump size, pain, and bowel habit changes.
What should be avoided?
- Do not assume all anal lumps are hemorrhoids.
- Do not use strong topical steroid creams for long periods without advice.
- Do not try to cut, squeeze, burn, or tie off a protruding lesion.
- Do not delay evaluation for recurrent bleeding.
- Do not ignore anemia, weight loss, or bowel habit changes.
| Feature | Anal polyp | Hemorrhoid |
|---|---|---|
| Main structure | Mucosal tissue growth | Enlarged vascular cushion or swollen vein |
| Common trigger | Irritation, inflammation, or polyp disease | Constipation, straining, pregnancy, pressure |
| Pain | Often painless unless irritated | Can be painful, especially external thrombosis |
| Bleeding | May occur; should be evaluated | Common, often bright red |
| Diagnosis | Examination, anoscopy, sometimes colonoscopy/pathology | Examination, anoscopy, grading if internal |
| Treatment | Monitoring or removal depending on features | Lifestyle, medication, office procedures, laser, surgery |
What Are the Medical Treatment Options?
Medical treatment depends on the diagnosis. Treating a polyp as a hemorrhoid, or a hemorrhoid as a harmless lump, can delay the correct approach. A proctology examination helps decide whether anoscopy, rectoscopy, colonoscopy, biopsy, removal, hemorrhoid grading, or other tests are needed.
Anal polyp evaluation and treatment
Anal or rectal polyps may be monitored, removed, or sent for pathology depending on size, appearance, symptoms, location, and patient risk factors. If the lesion is suspected to be a colorectal polyp, colonoscopy may be recommended. Mayo Clinic notes that colon polyps often do not cause symptoms, but early detection and removal can be important because some types may become cancerous over time.
Hemorrhoid treatment
Hemorrhoid treatment depends on the type and grade. Mild cases may improve with stool regulation, fiber, hydration, and topical symptom relief. Internal hemorrhoids that persist may be treated with rubber band ligation, sclerotherapy, infrared coagulation, laser hemorrhoid treatment, or surgery. ASCRS hemorrhoid guidance includes office-based procedures for many grade I-II and selected grade III internal hemorrhoids that do not respond to medical therapy.
When colonoscopy may be needed
Colonoscopy may be considered if bleeding is persistent, if there are risk factors for colorectal polyps or cancer, if the patient is within screening age, or if symptoms include anemia, bowel habit changes, unexplained weight loss, or family history. The goal is not to alarm every patient, but to avoid missing disease beyond the anal canal.
When Are Laser or Modern Treatments Preferred?
Laser or modern treatments may be considered for hemorrhoids when symptoms persist despite conservative care, when internal hemorrhoids prolapse or bleed, or when the patient is suitable for a minimally invasive approach. Laser hemorrhoid treatment targets hemorrhoidal tissue and blood flow, aiming to reduce swelling and symptoms in selected patients.
Laser is not a treatment for every anal polyp. Polyps generally require identification, removal, pathology, or monitoring depending on their type. If a protruding lesion is actually a polyp, choosing a hemorrhoid procedure without diagnosis would be the wrong road in the maze.
What Is Recovery Like After Treatment?
Recovery depends on the treatment method and diagnosis. Small hemorrhoid procedures may allow return to daily life relatively quickly, while surgery may require more downtime. Polyp removal recovery depends on location, size, removal method, and whether pathology review is required.
After hemorrhoid treatment
- Mild discomfort, pressure, or small bleeding may occur after some procedures.
- Constipation prevention is important.
- Straining and long toilet sitting should be avoided.
- Follow-up depends on hemorrhoid grade and treatment type.
After anal or rectal polyp removal
- Recovery varies by removal technique.
- Pathology results may guide follow-up.
- Further colonoscopy may be needed if colorectal polyps are suspected.
- Bleeding, fever, worsening pain, or heavy discharge should be reported.
What Should Definitely Not Be Done?
Anal symptoms are easy to underestimate. The danger is not panic; the danger is guessing. Guesswork can turn a treatable problem into a delayed diagnosis.
- Do not self-diagnose a lump as hemorrhoids without examination.
- Do not ignore recurrent rectal bleeding.
- Do not use over-the-counter hemorrhoid creams for weeks without improvement.
- Do not attempt to remove, cut, tie, or burn anal tissue at home.
- Do not delay care if bleeding appears with bowel habit changes.
- Do not assume painless bleeding is harmless.
- Do not skip recommended colonoscopy if risk factors are present.
- Do not stop follow-up after polyp removal if pathology requires surveillance.
When Should You See a Doctor?
You should see a proctology specialist if you have persistent bleeding, a new anal lump, mucus discharge, itching that does not improve, pain, prolapse, or a change in bowel habits. A short examination can often separate hemorrhoids from polyps, fissures, fistulas, skin tags, warts, prolapse, or other conditions.
Medical evaluation is especially important if you have:
- Recurrent rectal bleeding
- A palpable lump inside or outside the anus
- Bleeding without pain
- Mucus discharge or unexplained wetness
- Rapidly growing or changing tissue
- Family history of colorectal cancer or polyps
- Unexplained anemia or fatigue
- Change in bowel habits
- Unexplained weight loss
Frequently Asked Questions About Anal Polyps and Hemorrhoids
Are anal polyps and hemorrhoids the same thing?
No. Anal polyps and hemorrhoids are not the same thing. Anal polyps are tissue growths from the lining of the anal canal or rectum. Hemorrhoids are enlarged vascular cushions or swollen veins around the anus and lower rectum. They may both cause bleeding, itching, mucus, or a lump sensation, but their structure and treatment are different. A physical examination, anoscopy, and sometimes colonoscopy or pathology review may be needed to make the distinction safely.
Can an anal polyp be mistaken for hemorrhoids?
Yes. An anal polyp may be mistaken for hemorrhoids because both can feel like a protrusion or lump near the anus. The confusion becomes more likely when there is bright red bleeding, mucus, itching, or fullness. However, hemorrhoids are vascular structures, while polyps are tissue growths. Their treatment is different. A hemorrhoid may be treated with lifestyle changes or office procedures, while a polyp may need monitoring, removal, or pathology review. Self-diagnosis is not reliable.
Which causes more bleeding: polyps or hemorrhoids?
Hemorrhoids commonly cause bright red bleeding during or after bowel movements, especially internal hemorrhoids. Polyps can also bleed, but many polyps cause no symptoms at all. The amount of bleeding alone cannot reliably distinguish the two. Painless bright red bleeding may still need evaluation, especially if it recurs, appears with bowel habit changes, or occurs in someone with a family history of colorectal cancer or polyps. It is safer to identify the source rather than guess from the bleeding pattern.
Are anal polyps dangerous?
Many anal or inflammatory polyps are benign, but not every polyp should be ignored. Some rectal or colorectal polyps may have precancerous potential depending on type, size, and microscopic features. This is why removal and pathology review may be recommended in selected cases. Danger does not come from the word “polyp” alone; it comes from not knowing what type of tissue it is. Rapid growth, bleeding, bowel habit changes, anemia, or family history should prompt medical evaluation.
Can hemorrhoids turn into polyps or cancer?
Hemorrhoids do not turn into polyps or cancer. They are swollen vascular cushions, not precancerous tissue growths. However, hemorrhoids can cause symptoms that resemble other conditions, including polyps and colorectal cancer. This is why recurrent bleeding should not be automatically blamed on hemorrhoids. A patient can have hemorrhoids and another condition at the same time. If symptoms persist, change, or do not respond to treatment, a specialist examination and sometimes colonoscopy may be needed.
How are anal polyps diagnosed?
Anal polyps are usually diagnosed with a proctology examination. The physician may inspect the anal area, perform a digital rectal examination, and use anoscopy or rectoscopy to see inside the anal canal. If the polyp appears higher in the rectum or if there are risk factors, colonoscopy may be recommended. If a lesion is removed, pathology examination can determine its exact type. This is important because treatment and follow-up depend on whether the lesion is inflammatory, fibroepithelial, adenomatous, or another type.
How are hemorrhoids diagnosed?
Hemorrhoids are diagnosed through history and examination. External hemorrhoids can often be seen during inspection. Internal hemorrhoids may require anoscopy and grading based on prolapse. The physician also checks for fissures, fistulas, skin tags, warts, polyps, abscesses, and other causes of bleeding or lumps. If bleeding is persistent, atypical, or associated with bowel habit changes, further tests may be recommended. Diagnosis should confirm the source of symptoms before treatment is chosen.
Do anal polyps need to be removed?
Not every anal polyp needs immediate removal, but many require evaluation. Removal may be recommended if the polyp bleeds, grows, causes symptoms, has suspicious features, or needs pathology confirmation. Some small inflammatory polyps may be monitored, while colorectal-type polyps are often removed because pathology matters. The decision depends on appearance, location, symptoms, patient age, family history, and colonoscopy findings when relevant. A physician should decide whether observation, removal, biopsy, or further testing is appropriate.
When should rectal bleeding be checked?
Rectal bleeding should be checked if it is recurrent, heavy, painless, mixed with stool, associated with mucus, or appears with bowel habit changes, anemia, fatigue, weight loss, or abdominal pain. It should also be evaluated if there is a family history of colorectal cancer or polyps. Even if the bleeding looks like typical hemorrhoid bleeding, it is safer to confirm the source. Many anal conditions can bleed, and some important diseases may be missed if all bleeding is assumed to be hemorrhoids.
5 Key Takeaways
- Anal polyps and hemorrhoids can look or feel similar, but they are structurally different conditions.
- Hemorrhoids are enlarged vascular cushions; anal polyps are tissue growths from the mucosal lining.
- Both conditions may cause bleeding, itching, mucus, or a lump sensation, so self-diagnosis is unreliable.
- Polyps may need removal or pathology review, while hemorrhoids are treated according to type and grade.
- Persistent rectal bleeding, bowel habit changes, anemia, rapid growth, or unexplained weight loss require medical evaluation.
Get Evaluated for Anal Lumps, Bleeding or Hemorrhoid-Like Symptoms
If you have rectal bleeding, a lump near the anus, itching, mucus discharge, or symptoms that do not improve, a proctology examination can help distinguish hemorrhoids from anal polyps and other conditions.
📞 Phone: +90 212 550 81 93
Related Articles
Hemorrhoids and anal lump topics
Similar symptoms and related conditions
Sources and References
- NIDDK — Symptoms and Causes of Hemorrhoids. Accessed May 1, 2026.
- NIDDK — Symptoms and Causes of Colon Polyps. Accessed May 1, 2026.
- Mayo Clinic — Colon Polyps: Symptoms and Causes. Accessed May 1, 2026.
- NHS — Piles / Haemorrhoids. Accessed May 1, 2026.
- ASCRS Toolkit — Management of Hemorrhoids, 2024. Accessed May 1, 2026.
- Dr. Yasir Gozu — Clinical experience and patient observations in proctology, Istanbul, 2005-2026.

Leave a reply